What is it?
Coeliac disease (pronounced ‘seel-ee-ak’ and spelt celiac in some countries) is a common but under-diagnosed immune-based condition, triggered by gluten. In those with coeliac disease, the body’s immune system reacts to gluten by attacking itself. The resulting inflammation can lead to many different symptoms.


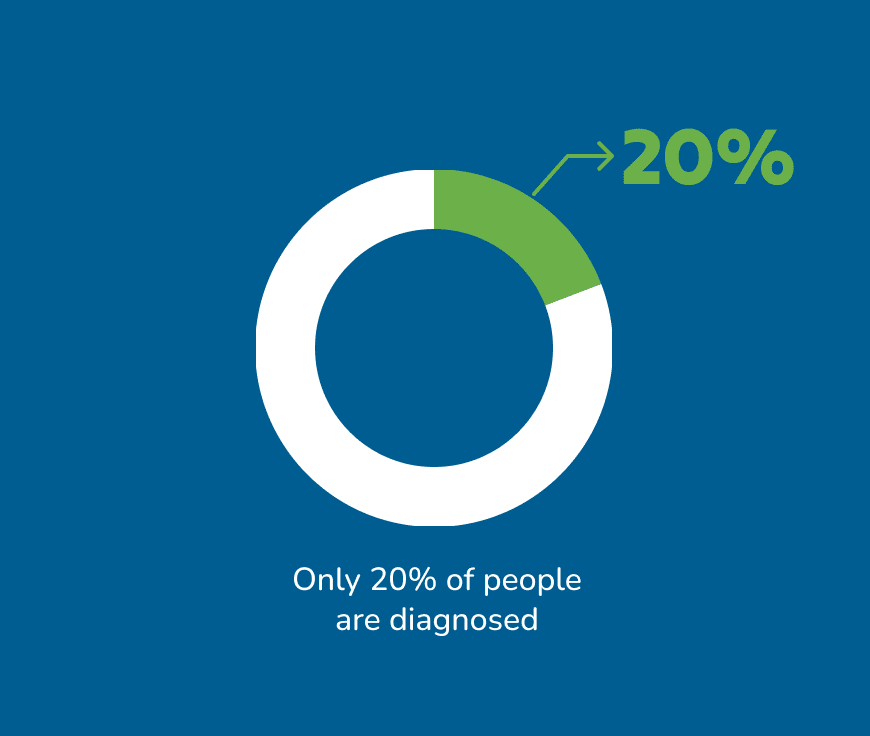

Approximately 1 in 70 Australians have coeliac disease. However, only 20% of this number are diagnosed. This means the vast majority of Australians who have coeliac disease don’t yet know it.
Long term health problems, such as osteoporosis, liver disease, infertility and a higher chance of developing other autoimmune conditions, can occur if a diagnosis of coeliac disease is overlooked or delayed. A diagnosis of coeliac disease and treatment with the gluten free diet reduced the risk of any long term complications.
Who can get coeliac disease?
Coeliac disease is a disease that can develop at any age. It affects both men and women of all ethnicities.
Both genetic and environmental factors are important in coeliac disease development.
As a genetic condition, you must be born with certain genes (HLA type) to be able to get coeliac disease (having the HLA genes means you are ‘genetically predisposed’). But this is not the end of the story… most people with the ‘coeliac genes’ will never develop coeliac disease. The HLA genes are common, carried by around 50% of Australians, however only 1:40 HLA carriers will get coeliac disease.
Environmental factors play an important role in triggering coeliac disease to develop in those who are ‘genetically predisposed’.
Fact sheets


Coeliac Disease


Conditions associated with Coeliac Disease
How do you treat coeliac disease?
Everyone diagnosed with coeliac disease must follow a gluten-free diet; this is the only treatment for coeliac disease. Following a gluten free diet allows the body to heal and symptoms to resolve.
Coeliac disease is a lifelong diagnosis; if gluten is reintroduced to the diet, relapse will occur.
Is coeliac disease different to non-coeliac gluten sensitivity?
‘Non-coeliac gluten sensitivity’, or gluten intolerance, describes a set of symptoms people attribute to dietary gluten, but the cause and treatment is not well understood. Irritable Bowel Syndrome (IBS) is a diagnosis that can be considered once coeliac disease and other medical diagnoses have been excluded. IBS is common and its symptoms can mimic those of coeliac disease; however, unlike coeliac disease, it does not cause an immune response or inflammation. Dietary modification (in combination with other treatments) is often the first line of therapy for IBS. While gluten is often blamed, the malabsorption of fermentable sugars (FODMAPs) is a more likely cause in those with IBS.
Importantly, only once coeliac disease and other medical conditions have been excluded should other dietary triggers for symptoms be explored. Feeling better when you remove wheat or gluten from your diet does not necessarily mean you have coeliac disease. You should consult with your doctor to investigate all potential causes for your symptoms.
Please note: There is no ‘test’ to diagnose IBS or gluten intolerance.















